RENDEL, Haiti: There is a plague on this town.
Even before the winds and rain toppled nearly everything standing, cholera was already here. It came down from the mountains, washing into the lives of the thousands who once lived above the river.
Now the only sign of life is in a makeshift clinic dealing with hundreds of suspected cholera cases, a small concrete building where just a few nurses contend with the swarms of patients arriving every hour.
There is only one public official left. The mayor was struck by cholera and left on foot to seek treatment hours away. One deputy died of the disease last week. Another fled, like so many others, to escape the ruin visited on the town of Rendel by Hurricane Matthew and its aftermath.
“Ninety per cent of our village is gone,” said Eric Valcourt, a priest in the Roman Catholic parish that runs the clinic and a school that now serves as a shelter for those too sick or poor to leave. “Many left by foot to escape the disease and devastation. The rest died from cholera or the hurricane.”
A week has passed since the hurricane tore through this remote stretch of Haiti’s southern peninsula, leaving an apocalyptic landscape of treeless countryside, disarticulated homes and a land robbed of its natural riches.
But for many, the torment has only started. Cholera, the disease at the heart of Haiti’s last disaster, is being spread again by this one.
About 10,000 people have died and hundreds of thousands have been sickened since cholera first appeared in late 2010. Scientists say it was brought to Haiti by UN peacekeepers stationed at a base that leaked waste into a river. After years of deflecting blame, the United Nations this summer acknowledged “its own involvement” in the suffering Haiti has experienced from the disease.
Now, cholera is stalking the areas gutted by the hurricane, a long peninsula of coastal towns and mountain villages where clean water was already hard to find, long before the storm. Here in the remote town of Rendel, a gruelling four-hour trek to the nearest paved road, the disease has spread to every crevice of this valley and the hills above.
“We are all at risk,” said the last official in Rendel, Pierre Cenel, the magistrate.
The town of Rendel and its surroundings, which once sheltered 25,000 people, are the epicentre of a potential disaster. Thousands have left on foot, fording a waist-high river that bends so often that it requires nine crossings along the way. The things they carry are all they have left: split bags of clothes and small livestock. They carry disease, too, destined for towns connected to the rest of the country by road.
One family braced for a river crossing, the youngest daughter in a purple dress with a pink sweater, clutching a live chicken in her arms.
“I don’t know what we will do, but we can’t live here,” said her father, Donald Augustin, 37, balancing a black suitcase on top of his head. “The people are dying of cholera.”
Those who remain bear witness to the slow release of misery. Heroic nurses care for patients splayed on the floor like rag dolls, some resting atop the improvised stretchers they arrived on. Patients vomit and defecate on the floor or into small yellow buckets, too sick to leave their stifling confines. The waste is emptied into a hole on the hill just behind the clinic, awaiting the next rainfall to overflow once again. The smell of bile and excrement stings the nostrils.
Patients come and go to escape the stench and the oppressive heat, while relatives risk disease to tend to their loved ones. Many refuse to come to the clinic at all, fearful of being blamed for the outbreak. Sick people midway through their recoveries are shown the door to make way for new patients. A single lantern is the only light for the nurses to work by during gruelling 12-hour shifts.
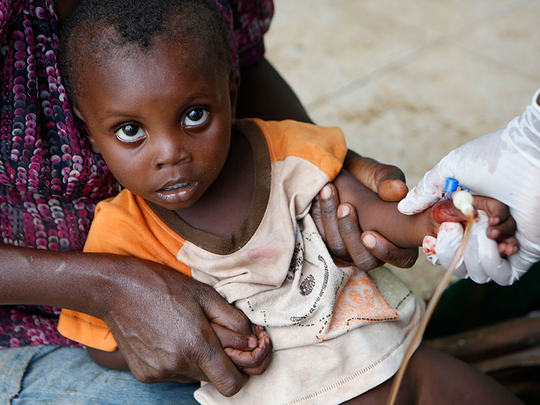
A lowing child is rocked on her mother’s lap as an IV drip pumps fluids into her tiny arm. A young husband feeds his pregnant wife hot porridge, blowing over each spoonful as patients writhe beside and beneath them. A father kisses the ear of his four-year-old son to soften the taste of saline solution.
“I spent the night here with her but the bed is too small for both of us so I slept outside and checked on her every hour,” said Jean Romit Cadet, 22, the young husband, handing the spoon to his wife and urging her to eat. “If I get sick, I get sick. I’m responsible for her.”
One morning this week, a rush of patients poured into the clinic, some carried on stretchers. A nurse tried to register each patient but lost track in the chaos, unable to take down everyone’s details.
A young girl entered the clinic and told the head nurse she was suffering from diarrhoea.
“For how many days?” the nurse asked.
“Three,” the girl replied.
“Why are you only coming now?” the nurse demanded. “We need to hook you up to an IV.”
The girl refused.
“I’m not vomiting,” she yelled over her shoulder as she left the clinic.
The nurse turned to the crowd in the entrance of the clinic, a porch robbed of its roof by the storm. In its place hung a sagging blue tarp.
“This is the problem,” she told the crowd of patients, parents holding sick children and others laid out on the floor, their eyes lolling back into their heads. “She doesn’t want to use the IV because she isn’t vomiting. But that doesn’t mean she doesn’t have cholera.”












